The Most Advanced
Technology
FOR GREAT EYE CARE

Comprehensive
Eye Exams

Children's and
Senior’s Exams
Medical
Eye Care

Dry Eye
Treatments
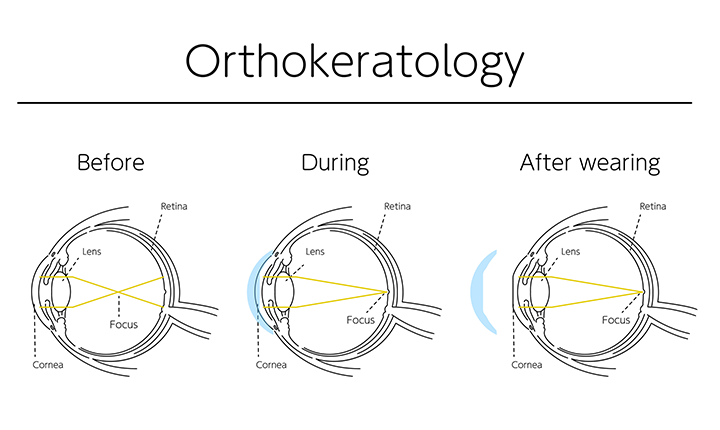
Myopia
Control

Computer Vision
Syndrome

Specialty Contact
Lenses

Binocular Vision and Vision Therapy
Diagnosing and Treating Eye Diseases and Problems in West Vancouver, Squamish and Powell River
Optomeyes Eye Care is based in 3 locations to better serve you. Find us in West Vancouver, in Squamish and Powell River to benefit from our award-winning eye care services. We dedicate ourselves to providing high quality, personalized comprehensive eye exams, specialized eye exams for children and seniors, as well as a variety of advanced eye care services listed below:
- Comprehensive Eye Exams for all ages
- Prescription Eyeglasses and onsite Lab
- Advanced Medical Diagnostic Imaging
- Ocular Disease Treatment
- Dry Eye Center with Lipiflow Thermal Pulsation IPL and RF
- Laser Refractive Cataract Surgery
- Myopia Control Orthokeratology
- Macular Degeneration Risk Consultation Genetic Testing
- Pediatric Eye Care
- Large Optical with Eyeglass Sunglass Frames
- Regular Specialty Contact Lenses
- Sports and Performance Vision
- Ocular Aesthetics
Legal Notice
The information below applies to all the information contained on the optomeyes.ca Website.
The users of this Website agree to comply with the terms set out below.
TERMS OF USE
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. owns and operates a Website at optomeyes.ca (hereinafter referred to as the “site” or “Website”). Optomeyes, West Vancouver, Squamish and Powell River British-Columbia.® trademark except as otherwise noted on the site, which is accessible to all users (hereinafter referred to as the “user” or “users”). Refrain from using this Website unless you agree to comply with the conditions.
RISKS ASSOCIATED WITH INFORMATION
Information on this Website is intended for informational purposes only and has no contractual value. Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. reserves the right to modify the content of this site. At any time, without prior notice. Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. assumes no liability for errors or omissions in the content of this Website or for information reliability or completeness of said information.
Information published on this Website is based on marketing, statistical or commercial services or other sources the Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. considers reliable and are the sole responsibility of their authors and not of Optomeyes, West Vancouver, Squamish and Powell River British-Columbia.. We do not assume any liability for the accuracy or completeness of said information and in no circumstance should this information be regarded as such. Opinions and information as presented on this site reflect our position as of the date of publication and are subject to change without notice.
UPDATING OF THE WEBSITE UNDER THE RESPONSIBILITY OF Optomeyes, West Vancouver, Squamish and Powell River British-Columbia.
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia., its employees and directors will not be liable for damages incurred as a result of the information published on this site, for the views and advice published, expressed or implied regardless of its nature.
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. expressly refuses any and all responsibility for the manner in which the user of the site may use the information contained, in any decisions that may be made and in the actions that may or may not be taken based on said information.
COPYRIGHT PROTECTION
Presentations made and contained on this site are the intellectual property of Optomeyes, West Vancouver, Squamish and Powell River British-Columbia.. Reproduction in whole or in part of this site on any other medium in prohibited without the express permission of Optomeyes, West Vancouver, Squamish and Powell River British-Columbia..
User may solely use the information contained on this site for personal use. Reproduction in whole or in part of said information on paper may only be performed for personal use. Said information is not to be copied, distributed or transmitted to third parties nor may it be inserted in a document or other medium.
HYPERTEXT LINKS
The links to external Websites and their content shall not be prejudged and Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. will in no way be held responsible for any direct or indirect prejudice that may result from gaining access to and usage of said sites.
CONFIDENTIALITY
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. draws the attention of the user to the fact that all communication transmitted through this Website remains in the public domain and not the private domain. OSI cannot accept responsibility for the security of the transmission of information.
The confidentiality and integrity of the information circulating over the internet cannot be ensured. Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. cannot accept responsibility in the case that data contained on this site is intercepted.
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. site uses cookies. These cookies are small text files saved on the hard disk of a user's computer. These files are completely harmless and cannot contain viruses. These cookies are used to analyze visits to the site. Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. calls upon Google Analytics to help track how users use the site. The number of visitors, path taken to access the site and length of each visit are measured. The cookies cannot, in any way, identify the user. All data is completely anonymous and compiled solely for the purpose of improving the site and tailoring the content to the needs of its visitors.
The person responsible for the protection of personal information is the owner of : Optomeyes, West Vancouver, Squamish and Powell River British-Columbia.
VIRUSES AND TECHNICAL GLITCHES
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. makes no representations that the content of this site is free of infections, viruses, worms, Trojan horses and/or other codes with contaminating or destructive properties. It is the user's responsibility to take protective measures.
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. DECLINES ALL RESPONSIBILITY IN THE EVENT OF ANY INTERRUPTION OR NON-AVAILABILITY OF THE SERVICE
Under no circumstances shall Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. be held responsible for transmission errors of any sort, such as loss of or damage to data, or changes of any type whatsoever, including direct or indirect damage resulting from the use of the services provided on this site.
JURISDICTION
This Agreement shall be governed by and construed in accordance with the laws of the province of BC.
Any dispute arising of this Agreement shall be brought before the court in the judicial district of
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia.'s head office.
Address:
204 - 1555 Marine Dr West Vancouver British-Columbia, V7V 1H9;
Tel: 604-922-0413.
PUBLISHING FIRM
Optomeyes, West Vancouver, Squamish and Powell River British-Columbia.
204 - 1555 Marine Dr West Vancouver British-Columbia, V7V 1H9
Tel: 604-922-0413
Acceptance of the Privacy Policy
Thank you for visiting optomeyes.ca (the “Website”), provided to you by Optomeyes, West Vancouver, Squamish and Powell River British-Columbia. (“We”). We respect the privacy of every individual who visits the Website and are sensitive to privacy issues on the Internet. We believe it is important that you know how we deal with information received about you.
This privacy policy (the “Privacy Policy”) explains how we collect, use, disclose, and protect the personal information of our customers and Website users ("you"), describes the types of information we may collect from you or that you may provide to us, and our practices for collecting, using, maintaining, protecting, and disclosing that information. The Website is for general audiences and is not specifically targeted to or intended for use by children.
We will only use your personal information in accordance with this Privacy Policy unless otherwise required by applicable law. We take steps to ensure that the personal information that we collect about you is adequate, relevant, not excessive, and used for limited purposes. Privacy laws in Canada generally define "Personal Information" as any information about an identifiable individual, which includes information that can be used on its own or with other information to identify, contact, or locate a single person.
By accessing or using the Website, you are accepting the practices described in this Privacy Policy, and you are consenting to our processing of your information as set out in this Privacy Policy. We may modify or update this Privacy Policy from time to time; if we change this Privacy Policy in a manner that materially impacts your privacy rights, we will provide a notice to you. Your continued use of the Website or our services after any modification to this Privacy Policy will constitute your acceptance of such modification. However, when required by law, we will confirm your consent to the revised Privacy Policy terms. This Privacy Policy is incorporated into and considered a part of the Website Terms and Conditions of Use, located here
What information we collect
We collect and use several types of information from and about you, including:
- Personal Information, that we can reasonably use to directly or indirectly identify you, such as your full name, email address, telephone number and any other identifier we may use to contact you online or offline.
- Non-personal information is information that does not directly or indirectly reveal your identity or directly relate to an identified individual, such as demographic information, or statistical or aggregated information. Statistical or aggregated data does not directly identify a specific person, but we may derive non-personal statistical or aggregated data from Personal Information. For example, we may aggregate Personal Information to calculate the percentage of users accessing a specific Website feature.
How we collect the information
Information You Provide to Us
The information we collect directly from you may include:
- Communicating with us: When you contact us about a customer service issue, Vision Entrepreneur services or to make other inquiries, we collect the content of those communications, as well as your full name, clinic name, email, phone number, city, province, and any additional information that allows us to answer your request.
Information We Collect While You Interact With Us Through Cookies and Other Automatic Data Collection Technologies
- Refer to Cookie Policy (here)
Information We Collect About You From Third Parties
- Refer to Cookie Policy (here)
How we use your information
We use your information, including your Personal Information, to manage our business and to maintain and develop commercial relationships with you. We will collect, use, and disclose such information only to the extent that is necessary for those purposes.
We use information that we collect about you or that you provide to us, including any Personal Information:
- To provide you with information, products, or services that you request from us.
- To fulfill the purposes for which you provided the information or that were described when it was collected, or any other purpose for which you provide it.
- To improve the Website, products or services, marketing, or customer relationships and experiences.
- To allow you to participate in interactive features, social media, or similar features on the Website.
- To measure or understand the effectiveness of the advertising we serve to you and others, and to deliver relevant advertising to you.
- In any other way we may describe when you provide the information.
- For any other purpose with your consent.
How we share your information
We will not rent or sell your information to third parties without your consent. We only share your data as specifically provided in this Privacy Policy.
Other Disclosures
In addition to any disclosure you may have consented to or permitted under the terms of this Privacy Policy, we may transfer your data, including Personal Information to third parties in the following limited circumstances:
- information you expressly consent to be shared;
- when relating to anonymized information (individuals cannot be identified by it);
- when you decide to make the information indexable by search engines, to share or to distribute the information to people or otherwise to make it available to the public;
- to satisfy any applicable law, regulation, legal process or enforceable governmental request within or outside your country of residence when we have a good faith belief that the law requires it;
- to enforce this Privacy Policy, the Terms, or an agreement, including investigation of potential violations thereof;
- to detect, prevent, or otherwise address fraud, security or technical issues, or protect the operations or you;
- to protect our rights, property or safety as well as yours, the public, or others;
- in connection with an acquisition, merger, change in control, debt financing, reorganization, sales of assets, bankruptcy or other change of our corporate structure or status; or
- as necessary in connection with the performance of requested services or solutions, or as otherwise appropriate in connection with a legitimate need.
How we store and secure your information
Information Security
We are committed to protecting the confidentiality, integrity, availability and privacy of your Personal Information. We have put appropriate physical, technological and procedural security measures in place designed to help prevent your Personal Information from being lost, used, modified or accessed in an unauthorized way, or improperly disclosed. Examples of such measures include restricted access to offices, training of personnel, using passwords and well-defined internal policies and practices. We also use encryption technology and Secure Socket Layers ("SSL") in all areas of the Website where your personal account information is required.
In addition, we limit access to your Personal Information to those employees, agents, contractors and other third parties who have a business need-to-know. They will be required to process your Personal Information only on our instructions and they are subject to an obligation of confidentiality. Our service providers are required to maintain adequate security protections in place designed to help safeguard your Personal Information and are not permitted to use it for any purpose other than fulfilling services to us.
If you have any questions about securing your personal data, please contact us in accordance with the “How to Contact Us” section below.
Information Retention
We will retain your Personal Information for as long as it is needed:
- to provide the products and services that you have requested;
- to communicate with you about a purchase or a request you have made to us;
- to manage your choices and rights you have exercised pursuant to this Privacy Policy;
- to comply with our legal and regulatory obligations and to demonstrate compliance,
- to resolve disputes and to enforce our rights and agreements.
We may retain non-personal information that has been sufficiently aggregated or anonymized for a longer period.
Once the retention period is over, we will dispose of your Personal Information as provided for in our internal data retention and disposal policy.
Where We Store Information
We use facilities operated by "Amazon Web Services" and located in Canada as our information storage and processing infrastructure. Our service providers can also, from time to time, store your Personal Information in accordance with purposes outlined in this Privacy Policy.
How to contact us
If you have any questions about this Privacy Policy, you can contact us at 604-922-0413.